Medical Student Discussion Forum: How Peer Clinical Case Discussions Improve Learning

It is late evening after clinical postings.
A small group of medical students sits around a table in the hostel common room. One of them opens a notebook and reads aloud.
“52 year old male. Sudden onset chest pain. Sweating. Pain radiating to the left arm.”
The first answer comes quickly.
“Myocardial infarction.”
Someone nods.
Another student pauses and asks quietly.
“But what else could cause this?”
For a few seconds the room becomes thoughtful. Someone mentions aortic dissection. Another brings up pulmonary embolism. A third student starts questioning the history again. The case that looked simple a moment ago begins to open in different directions.
Conversations like this are common among medical students. They happen after ward rounds, in library corners, in hostel rooms, and increasingly inside a medical student discussion forum where learners from different institutions exchange clinical cases and reasoning.
These discussions often do something that solving a case alone cannot do.
They force students to explain why they think a diagnosis is correct, listen to how others approach the same case, and recognize gaps in their own reasoning.
Over time, these small conversations become one of the most powerful ways medical students learn how to think through clinical problems.
This idea is explored more deeply in our guide on why clinical case discussion improves diagnostic thinking for medical students, which explains how discussion helps shape diagnostic reasoning during training.
In this article, we focus specifically on how peer conversations, especially inside a medical student discussion forum, help strengthen that learning process.
Why Do Medical Students Discuss Clinical Cases With Peers?
Clinical medicine is rarely learned in isolation.
A student may read a case, identify the most likely diagnosis, and move on. The answer may even be correct. But the reasoning behind that answer often remains untested.
When the same case is discussed with peers, the learning process changes.
One student may focus on the presenting symptom. Another may question the timeline of the illness. Someone else may ask why certain diagnoses were excluded. Each perspective introduces a slightly different way of approaching the same clinical problem.
These conversations are common in study groups, after ward rounds, and increasingly within a medical student discussion forum, where learners share cases and compare how they interpret the same clinical information. These discussions form the foundation of what educators often describe as clinical case discussion learning, where reasoning develops through dialogue rather than memorization.
Several educational studies in medical training show that peer discussion and collaborative learning improve engagement, critical thinking, and diagnostic reasoning. When students explain their reasoning to others, they are more likely to identify gaps in their understanding and refine their clinical thinking.
There are a few reasons why this learning behavior appears naturally among medical students.
Clarifying reasoning
When explaining a diagnosis to peers, students must articulate how they moved from symptoms to conclusions. This process often reveals assumptions that were not obvious while solving the case alone.
Comparing interpretations
Different students notice different details in the same case. One may focus on risk factors, another on the progression of symptoms. Hearing multiple interpretations exposes learners to alternative diagnostic pathways.
Testing diagnostic thinking
A peer may challenge a diagnosis with a simple question:
“Why not consider another possibility?”
These small challenges encourage students to revisit their reasoning and consider broader differential diagnoses.
Over time, repeated case discussions help students develop a habit that is central to clinical practice: thinking through a problem from multiple perspectives before settling on a diagnosis.
What Happens When Clinical Cases Are Discussed Instead of Solved Alone?
Solving a clinical case individually is a common way students practice diagnostic reasoning. A student reads the history, reviews the symptoms, and arrives at the most likely diagnosis. If the answer matches the expected diagnosis, the case often feels complete.
But something important may still be missing.
When clinical cases are discussed with peers, the learning process becomes more visible. Instead of focusing only on the final diagnosis, the discussion shifts toward how each person arrived at their conclusion.
Three important changes usually happen during these discussions.

Reasoning becomes explicit
When a student solves a case alone, much of the reasoning remains internal. The diagnostic path may rely on intuition or pattern recognition. During a discussion, however, students must explain their thought process step by step. This explanation often reveals gaps or assumptions that were not obvious before.
Alternative diagnoses appear
Different students may interpret the same case in different ways. One student may prioritize the most common diagnosis, while another may notice details that suggest a less obvious possibility. These alternative interpretations expand the differential diagnosis and encourage a broader clinical perspective.
Blind spots become visible
Every learner develops cognitive shortcuts while solving cases. Sometimes these shortcuts lead to premature conclusions. When peers question a diagnosis or suggest a different explanation, these blind spots become easier to recognize.
Research in medical education suggests that collaborative discussion and peer learning can strengthen critical thinking and improve the way students approach clinical problems, particularly when learners explain and challenge each other's reasoning.
For many students, this is why discussing cases with peers gradually becomes a natural part of learning. A case that seemed straightforward when solved alone often becomes more instructive when explored from multiple viewpoints.
How Peer Case Discussions Improve Diagnostic Reasoning
Diagnostic reasoning develops gradually. It improves not only by solving more cases, but by examining how those cases are interpreted.
When clinical cases are discussed with peers, the reasoning behind a diagnosis becomes visible. Students begin to observe how others connect symptoms, prioritize findings, and narrow down possible diagnoses. Over time, this shared process strengthens the way clinical problems are approached.
Several mechanisms explain why peer case discussions help develop stronger diagnostic reasoning.
Revealing Hidden Assumptions
When students first approach a clinical case, they often form an early impression of the diagnosis. This initial idea can shape how the rest of the information is interpreted.
During peer discussion, another student may ask a simple question about that assumption:
“Why do you think this symptom points to that diagnosis?”
Explaining the reasoning forces the student to examine whether the assumption is supported by the clinical details or whether it was formed too quickly. This process helps learners recognize when early conclusions influence later interpretation of the case.
Identifying Reasoning Gaps
While presenting a case to peers, students often realize that parts of their reasoning are incomplete. For example, they may know the final diagnosis but struggle to explain why alternative diagnoses were excluded.
Discussion makes these gaps easier to notice. When peers ask questions about investigations, timelines, or risk factors, students are encouraged to revisit the clinical logic that connects each step of the case.
Refining Differential Diagnosis
Clinical reasoning improves when students actively compare multiple diagnostic possibilities rather than focusing on a single answer.
In peer case discussions, different students may propose different explanations for the same presentation. One may consider a common diagnosis, while another suggests a less frequent but plausible alternative. This exchange expands the differential diagnosis and encourages more systematic evaluation of possibilities.
Learning From Different Clinical Perspectives
Each student brings a slightly different experience to a case discussion. Some may recall similar cases from clinical postings. Others may focus on textbook knowledge or pathophysiology.
When these perspectives come together, students are exposed to multiple ways of approaching the same clinical problem. Over time, this exposure helps learners build a broader and more flexible diagnostic framework.
Educational research in medical training has shown that collaborative case discussions and peer learning can improve critical thinking and diagnostic reasoning, especially when learners explain and challenge each other’s interpretations.
For many medical students, repeated discussions like these gradually shape how they think through clinical cases. Instead of relying only on the first diagnosis that comes to mind, they learn to examine assumptions, compare possibilities, and refine their reasoning step by step.
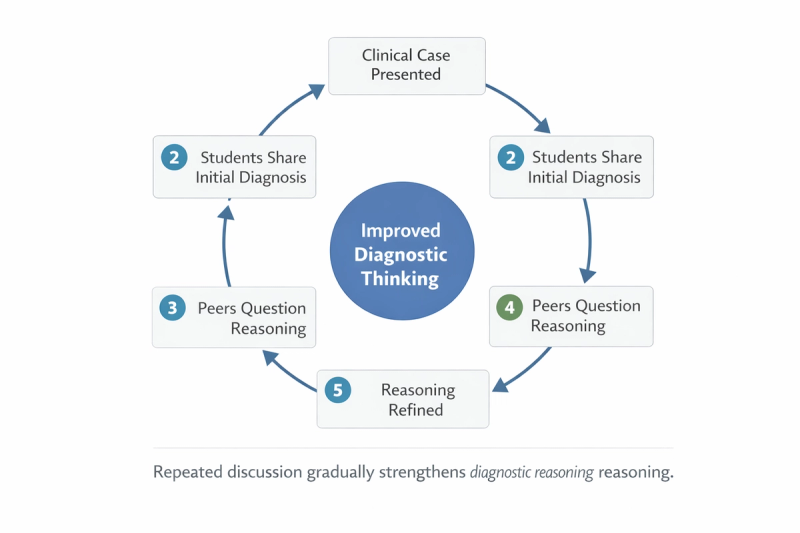
Where Medical Students Usually Discuss Clinical Cases
Clinical case discussions happen in many informal and structured settings during medical training. These environments allow students to compare reasoning, question interpretations, and learn from each other's perspectives.
Several common spaces naturally function as a medical student discussion forum, even if they are not formally labeled that way.
Each of these environments functions as a practical medical student discussion forum, where clinical reasoning develops through shared analysis of patient cases.

Ward Rounds
During ward rounds, students often discuss patient cases with residents and consultants. Questions about diagnosis, investigations, and management create short but valuable moments where clinical reasoning is openly examined.
Small Group Learning Sessions
Many medical schools use case based or problem based learning sessions. In these settings, students analyze clinical cases together, explain their reasoning, and build differential diagnoses collectively.
Peer Study Groups
Outside formal teaching environments, students frequently review clinical cases with friends or classmates. These discussions are often more relaxed and allow learners to explore different diagnostic ideas without the pressure of evaluation.
Online Discussion Forums
Increasingly, students also discuss clinical cases through digital platforms where learners from different institutions can share cases, ask questions, and compare clinical reasoning. Platforms designed specifically for medical learners, such as MedCoterie, aim to recreate this collaborative environment online by allowing students to explore clinical cases together and learn from different perspectives.
Why Discussion Often Teaches More Than Passive Case Reading
Reading clinical cases is a common way medical students study. It exposes learners to different presentations and diagnoses. However, simply reading a case often leads to recognizing the answer rather than understanding the reasoning behind it.
Discussion changes this learning process in important ways.
Active recall
When students discuss a case, they must retrieve relevant knowledge from memory instead of simply recognizing it on the page. Recalling symptoms, mechanisms, and possible diagnoses strengthens long term understanding.
Reasoning articulation
Explaining a diagnosis to peers requires students to describe how they moved from symptoms to conclusions. This process makes their reasoning clearer and often exposes assumptions or incomplete explanations.
Collaborative problem solving
Different students approach the same case with different perspectives. When these perspectives are shared, the group collectively explores multiple possibilities and evaluates them together. This collaborative process often leads to deeper clinical insight than reading the case alone.
Because of these mechanisms, discussing clinical cases with peers often turns a simple learning exercise into a more active process of analyzing, questioning, and refining diagnostic reasoning.
The Risks of Case Discussions Without Structure
While discussing clinical cases with peers can improve learning, the process is not always reliable without some structure.
When case discussions happen informally, a few common problems may appear.
Incorrect reasoning spreading
If a diagnosis is explained incorrectly and no one challenges it, the reasoning may be accepted by the group. Without verification or guidance, misunderstandings can spread quickly within peer discussions.
Dominance by confident students
In many discussions, one or two confident voices may influence the direction of the conversation. Other students may hesitate to question them, even when they notice inconsistencies in the reasoning.
Superficial discussion
Sometimes case discussions stop at identifying the final diagnosis. The group may not explore why alternative diagnoses were excluded or what clinical details were most important in reaching the conclusion.
Because of these limitations, effective case discussions usually benefit from a simple structure that encourages students to explain their reasoning, examine alternatives, and question conclusions carefully.
How to Make Peer Case Discussions Actually Improve Learning
Peer case discussions become more valuable when they follow a simple structure. Without some discipline, conversations may drift toward quick answers instead of careful reasoning.
A few practical habits can make these discussions far more effective for learning.
Structured case presentation
Start by presenting the case clearly. Include the patient’s age, main complaint, relevant history, examination findings, and key investigations. A structured presentation helps everyone analyze the same clinical information.
Reasoning explanation
Instead of stating only the final diagnosis, students should explain how they reached it. Describing the reasoning path helps others understand the logic behind the conclusion.
Asking diagnostic questions
Peers should actively question each step of the reasoning. Asking why certain diagnoses were considered or excluded encourages deeper analysis of the case.
Comparing differential diagnoses
Rather than focusing on a single answer, the discussion should explore multiple possible diagnoses. Comparing these options helps students evaluate clinical clues more carefully.
When discussions follow these practices, they move beyond guessing the diagnosis and become an opportunity to examine how clinical reasoning actually works.
Why Discussion Forums May Become Central to Medical Learning
Medical training has traditionally relied on discussions within a single classroom or hospital. While these environments are valuable, they often limit students to the clinical exposure and perspectives available in one institution.
Discussion forums are gradually expanding this learning environment.
Cross institution discussion
When students from different colleges discuss clinical cases together, they are exposed to varied teaching styles, patient populations, and diagnostic approaches. This broader interaction helps learners see how the same clinical problem may be interpreted differently.
Diverse clinical exposure
Not every student encounters the same cases during clinical postings. Discussion forums allow learners to explore cases shared by peers, increasing exposure to a wider range of clinical presentations.
Collaborative reasoning culture
Regular discussion encourages students to question assumptions, compare diagnostic ideas, and refine their reasoning together. Over time, this creates a culture where clinical thinking develops through shared exploration rather than isolated study.
As medical education increasingly integrates digital learning spaces, platforms designed for structured case discussions, such as MedCoterie, may help extend this collaborative reasoning culture beyond individual classrooms and hospitals.
Clinical reasoning develops gradually through exposure, reflection, and discussion. While solving cases individually builds familiarity with diagnoses, discussing them with peers reveals the thinking behind those diagnoses. Over time, these conversations help medical students move from recognizing answers to understanding clinical reasoning.
References
- McLean, S. F. (2016). Case-Based Learning and Its Application in Medical and Health-Care Fields: A Review of Worldwide Literature.
Journal of Medical Education and Curricular Development.
https://pmc.ncbi.nlm.nih.gov/articles/PMC5736264/
Case-based learning uses real clinical scenarios to help students connect theoretical knowledge with practical clinical reasoning. - Koenemann, N., et al. (2020). A Novel, Supervised Peer-Teaching Format to Promote Clinical Reasoning Through Clinical Case Discussions.
https://pmc.ncbi.nlm.nih.gov/articles/PMC7499459/
Structured peer-led case discussions can strengthen clinical reasoning by allowing students to collaboratively analyze diagnostic decisions. - Bruen, C., et al. (2025). Medical Student Experiences of Case-Based Learning in Medical Education.
https://pmc.ncbi.nlm.nih.gov/articles/PMC11781049/
Case-based learning encourages active participation, discussion, and problem solving, helping students develop clinical reasoning and decision-making skills. - Levin, M., et al. (2016). Teaching Clinical Reasoning to Medical Students Using Case-Based Approaches.
https://pmc.ncbi.nlm.nih.gov/articles/PMC6464440/
Structured case discussions help students develop diagnostic reasoning by encouraging analysis of symptoms, differential diagnoses, and problem representation. - Nunnink, L., et al. (2020). Peer-Assisted Learning in Simulation-Based Medical Education.
https://pmc.ncbi.nlm.nih.gov/articles/PMC8936843/
Peer-assisted learning allows students to teach and learn from one another, improving engagement and clinical problem-solving skills. - Li, Z., et al. (2025). Effectiveness of Peer-Assisted Learning in Medical Education: A Meta-Analysis.
https://pmc.ncbi.nlm.nih.gov/articles/PMC12404444/
Peer-assisted learning strategies often improve knowledge acquisition and practical clinical skills compared with traditional teaching methods.